Implementing Tracking Technology To Improve Infection Control

By Ari Naim, president and CEO of CenTrak
By the end of 2014, the World Health Organization estimated over 17,000 people had been infected with Ebola and over 6,000 have died. Worldwide, this deadly disease has cost approximately $32.6 billion over a two-year span. These data illustrate the critical need for effective and cost-efficient infection control measures but, in reality, few hospitals are equipped to prevent the spread of communicable diseases.
The Association for Professionals in Infection Control and Epidemiology distributed an Ebola readiness poll to 15,000 infection preventionists (IPs) and published the results in early 2015. Only 6 percent responded that their institutions were well-prepared to receive a patient with the Ebola virus. Methods to improve a hospital’s readiness according to IPs included:
- adding additional staff to support an infection prevention and control program
- providing healthcare workers with more training, and improving equipment and technology
Preventing Spread Of Disease With Real-Time Location System (RTLS)
RTLS is a valuable technological asset that can be implemented to provide instant tracking of healthcare staff, patients, and equipment, as well as help optimize the results of infection control and prevention programs and staff training. Strategic implementation of an RTLS system can improve a hospital’s readiness to protect patients, staff, and the surrounding community from an infectious disease outbreak.
To optimize the value of an RTLS system, specially trained hospital staff should be given the responsibility of utilizing the technology. IPs are preferably suited to this task but, although they are recognized as an important asset to infection control, over half of hospitals employ one or less IPs for their entire facility. These specialists are trained to collect, analyze, and interpret health data to plan prevention and intervention measures. They establish infection prevention policies and practices and ensure that they are appropriately implemented. The majority of hospitals could benefit from adding IPs to their staff as they are in a unique position to utilize an appropriately implemented RTLS system to prevent the spread of infections like Ebola.
Real-Time, Accurate Visibility With Use Of RTLS
IPs can use an RTLS system to improve compliance with infection control policies and practices (e.g., hand washing) to decrease the spread of disease. They can also track patients that may have a communicable disease and their interactions with hospital staff, other patients, visitors, and equipment. IPs also have the knowledge to properly collect, analyze, and interpret real-time data provided by the RTLS system in order to recognize and track trends, plan interventions, measure success, and report outcomes.
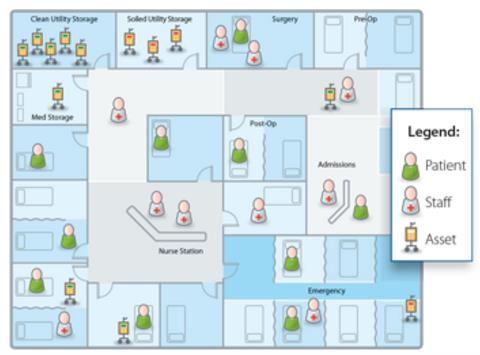
Floorplan graphic courtesy of CenTrak
Seamless, Automatic Integration Into EHR Systems
Most hospital staff, including IPs, complete their job duties through the use of an electronic health record (EHR) system. Hospitals that have adopted EHR systems use them to not only record data (e.g., patient chart) but also promote patient safety through the use of checklists, alerts, and predictive tools. EHR systems also allowed hospitals to streamline healthcare processes to improve patient care and outcomes. Overall, EHR systems are able to store detailed patient information over time and across care settings to help hospitals monitor, improve, and report data.
As hospitals have made the move to EHR systems, it is imperative that any new technology integrates with existing systems to maximize efficiency and cost-effectiveness through minimal interruption of day-to-day patient care and low staff training requirements. Seamless and automatic integration of RTLS into existing EHR systems can create a synergistic system that can track individual patients as well as larger units, such as the activity of a hospital floor, ward, or department. Integrated RTLS-EHR systems can also improve tracking of patient-provider interactions, use of equipment, and even the use of medication. This data can then be used to perform surveillance for infectious diseases and can alert hospitals of the potential for disease outbreak.

Reduction Of Infectious Disease Outbreaks
Infectious diseases like Ebola can have deadly consequences if they are allowed to spread uncontrollably, yet most hospitals are not prepared to handle a patient with Ebola. With the appropriate use of integrated, automatic RTLS technology, hospitals and their IPs can improve preparedness, increase infection control policy and compliance, and reduce infectious disease outbreaks.
